Heart disease, stroke and diet

To prevent or treat heart disease, you have to start on your plate.
Heart disease in all its forms is a major cause of death and disability worldwide. In the UK, around eight million people are living with a heart or circulatory disease and it causes a quarter of all UK deaths – that’s on average 480 deaths each day or one every three minutes. It is estimated that more than a half of the UK population, that’s every other person, will develop a heart or circulatory condition in their lifetime.
However, most cases are preventable or treatable with diet and lifestyle changes and this approach is more effective than drug therapy.
All major health institutions concerned with heart health agree on the same guidelines when it comes to prevention and treatment of heart disease which is a rare thing. These guidelines recommend a plant-based diet, low in saturated fat, salt, sugar and alcohol, and devoid of trans fats. This kind of diet should be centred around wholegrains, fruit and vegetables, pulses, nuts and seeds, include omega-3 fats, vitamins B12 and D, and may also include moderate amounts of tea and coffee.
Studies show that a wholefood vegan diet can be a true life-saver when it comes to heart disease, reducing the risk and helping to reverse atherosclerosis. On the other hand, diets based on meat, eggs, dairy, processed, fatty, salty and sugary foods are a recipe for a heart disaster. It’s not an overstatement to say that it’s not heart disease that runs in families, it’s just bad diet and lifestyle habits. Of course, there are genuine cases of genetic predisposition to cardiovascular diseases but those are much rarer than we tend to think.
The term heart disease is often used instead of cardiovascular disease (CVD) and describes a chronic disease of the heart and blood vessels. Closely related is cerebrovascular disease – a term which means the problem is in the vessels in the brain, greatly increasing the risk of stroke.
When the condition mostly affects the heart, not allowing enough blood into the arteries nourishing the heart muscle (coronary arteries), it’s called ischaemic or coronary heart disease.
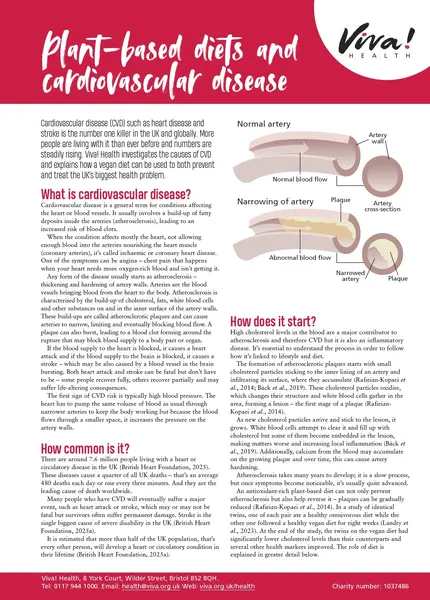
Any form of the disease usually starts as atherosclerosis – thickening and hardening of artery walls. Arteries are the blood vessels bringing blood from the heart to the body. Atherosclerosis is characterised by the build-up of cholesterol, fats, white blood cells and other substances on the inner surface of the artery walls. These build-ups are called plaques – atherosclerotic plaques – and can cause arteries to narrow, limiting and eventually even blocking blood flow. A plaque can also burst, leading to a blood clot forming around the rupture that may block blood supply to a body part or organ.
The first signs of heart disease risk may be chest pain (angina), shortness of breath, fatigue, palpitations or swelling in the legs, ankles or feet. In many cases, the first sign may be high blood pressure. The heart has to pump the same volume of blood as usual through narrower arteries to keep the body working but because the blood flows through a smaller space, it increases the pressure on the artery walls.
Some people have genes that make them more susceptible to heart disease, but lifestyle is what matters most. So, while risk factors such as family history, ethnic background and age are beyond your control, most of the risk factors listed below are heavily influenced by diet and lifestyle. For example, diets rich in meat increase the risk of high cholesterol, blood pressure and diabetes significantly, whereas diets rich in fruit, vegetables, pulses, wholegrains, nuts and seeds lower the risk. More often than not, it’s not about the genes that run in the family but about the diet and lifestyle that children inherit from their parents.
The main risk factors for heart disease include:
- high blood pressure – a risk factor but also often the first symptom, tightly linked to diet and lifestyle. For example, red and processed meat is linked to high blood pressure whereas fruit and vegetables lower it
- high cholesterol levels – the more cholesterol is in the blood, the more building material is available for plaque formation; the amount of cholesterol in the blood usually depends on the diet. For example, meat raises the risk; fruit and vegetables lower it
- smoking – the harmful substances resulting from tobacco smoking can damage blood vessels and increase plaque formation
- physical inactivity – the less we move about, the less exercise our circulatory system gets. For blood vessels to stay healthy, it’s important that they get stimulated by different levels of activity
- being overweight or obese – this factor has a lot to do with diet and physical inactivity. Again, diets packed with meat, high-fat dairy products and processed foods increase the risk and healthy plant-based diets lower it
- diabetes – having high blood sugar levels can directly damage blood vessels and it also increases cholesterol levels. There is a strong link between meat – especially red and processed meat – and diabetes, switching to plant-based sources of protein, such as pulses and nuts, lowers the risk
- alcohol consumption – excessive alcohol intake can increase your cholesterol levels and blood pressure, and contribute to weight gain
- family history – if your male relatives developed heart disease before the age of 55 and/or your female relatives developed it before the age of 65, it is considered a family history of heart disease
- ethnic background – in the UK, people of south Asian and Black African or African Caribbean background have an increased risk of heart disease
- age – the older we get, the higher the risk
- gender – men generally tend to develop heart disease at a younger age than women
Cholesterol is a waxy substance made by the liver and it’s normally used to build cell membranes and produce hormones, vitamin D and bile. Therefore, some cholesterol is necessary for healthy functioning of the body but the liver makes all we need. The problem starts when there’s too much of it.
Cholesterol doesn’t travel through the bloodstream on its own, it is carried with proteins and other fat molecules in special transport vehicles called lipoproteins. There are several types but the most important ones are:
- Low-density lipoprotein (LDL) – LDL is known as ’bad’ cholesterol because it distributes cholesterol to various tissues and is strongly associated with the build-up of atherosclerotic plaques
- High-density lipoprotein (HDL) – HDL is called ‘good’ cholesterol because it is the form of cholesterol in which it’s returned back to the liver for removal
High levels of cholesterol in the blood are a significant risk factor for developing heart and circulatory diseases. When total and LDL cholesterol levels are increased, there’s plenty of building material for atherosclerotic plaques to develop and grow. On the other hand, it’s good when HDL cholesterol levels are increased as that means cholesterol is being cleared away.
This table is a general guide for ideal cholesterol levels for healthy adults. If you have heart disease or diabetes, your target levels may be lower – your doctor will be able to advise you.
| mmol/L | mg/dL | |
| Total cholesterol | below 5.0 | below 193 |
| Non HDL cholesterol | below 4.0 | below 155 |
| LDL cholesterol | below 3.0 | below 166 |
| HDL cholesterol | above 1.0 for a man and above 1.2 for a woman | above 39 for a man and above 46 for a woman |
| Total cholesterol/HDL ratio | 6 or below | 6 or below |
Animals, just like us, make their own cholesterol and it’s a basic component of their cell membranes. So, all animal products – meat, fish, shellfish, eggs and dairy – contain cholesterol. Plant foods do not contain any cholesterol whatsoever, so a vegan diet is cholesterol-free.
Dietary cholesterol can have a different effect in different people – in some, it doesn’t affect blood cholesterol levels much but in others, it directly and significantly increases it. The range of how much cholesterol we absorb from the gut is 20 to 80 per cent.
However, even in people who have low-cholesterol-absorbing genes, dietary cholesterol can still increase blood cholesterol levels if consumed together with high amounts of saturated fat. Most animal products, such as meat, fish or high-fat dairy contain both, while others may be combined in a way that delivers both cholesterol and saturated fats in one meal – for example eggs with a buttered toast or chicken fried in butter, lard or coconut oil.
Plant-based diets based around wholegrains, fruit and vegetables, pulses, nuts and seeds and unsaturated fats have been shown time and again to be effective at keeping blood cholesterol levels down and at lowering them in people with high levels – vegan diets in particular. Read the research.
High blood pressure is closely linked with high cholesterol levels in the blood – it’s because cholesterol plaques in the arteries cause narrowing so the heart has to pump with an increased force to push blood through. High blood pressure always puts extra strain on blood vessels, the heart, brain, kidneys and eyes and increases the risk of blood vessel damage in these organs.
Many people aren’t aware of their cholesterol levels, so the first sign of heart disease risk may be a high blood pressure reading and only then do they find out they also have high cholesterol.
Among the main risk factors for high blood pressure (hypertension) are: being overweight, high salt intake, unhealthy diet, excessive alcohol and caffeine consumption, smoking, being older, genetics (some people naturally have higher blood pressure) and being of Black African, Black Caribbean or South Asian descent.
In most cases, medication alone isn’t able to lower both blood pressure and cholesterol levels to those considered as healthy so lifestyle modifications, including a diet based on plant foods, are essential to achieve meaningful risk reduction.
According to scientific studies, plant-based diets favouring wholegrains, fruit and vegetables, pulses, nuts, seeds and unsaturated fats lower your risk of high blood pressure and can effectively lower it when it’s too high. On the other hand, the more meat, salt, processed foods, sweets and saturated fat you eat, the higher your risk of hypertension. All this clearly points to a wholefood plant-based diet being the best at preventing high blood pressure and lowering it in people who have already developed it.
Across scientific studies, vegans consistently have been shown to have lower blood pressure than other diet groups and when compared with meat-eaters, for example, vegans may have up to a 63 per cent lower risk of high blood pressure.
Both prevention and disease can start in childhood. Research shows that children as young as three years may already have fatty patches in their blood vessels. As these children grow up, the fatty patches develop into atherosclerotic plaques, which is why people in their early twenties can have extensive atherosclerosis and suffer a sudden event.
From an early age, children can develop a number of cardiovascular risk factors, including high cholesterol levels, fatty streaks and even their first atherosclerotic lesions in the arteries, high blood pressure, high blood sugar levels and obesity. Being overweight or obese in childhood usually brings about other risk factors for heart disease and is an indicator of an unhealthy diet and lifestyle habits.
Children growing up on diets rich in meat and meat products, fat and sugar are more likely to have higher cholesterol, triglycerides and blood sugar levels and higher than healthy body weight, On the other hand, healthy childhood diets not only lower heart disease risk in adulthood but vegan children also have lower cholesterol levels and more antioxidants in the blood – this helps to protect their blood vessels and hearts even more. Read the research.
Establishing healthy dietary and lifestyle habits from an early age is important for cardiovascular health. Even though atherosclerosis can be reversed, it takes many years, so it’s best if it doesn’t develop in the first place.
Gut bacteria are usually beneficial and help us digest food and keep the gut healthy but there can also be harmful bacteria that produce toxic by-products, can damage the gut wall integrity and cause inflammation. What we eat determines which species thrive and which decline.
The beneficial gut bacteria thrive on fibre-rich foods (plant wholefoods) and produce a substance called butyrate and other short-chain fatty acids (SCFAs). These products serve as sources of energy for colonocytes (gut wall cells), help maintain healthy function of the gut wall, regulate gut pH and are anti-inflammatory. Other beneficial bacteria convert cholesterol into a substance called coprostanol, which is excreted with faeces – that way, these bacteria help to lower our cholesterol levels.
On the other hand, the potentially harmful gut bacteria thrive on meat, eggs, high-fat and fried foods, processed foods, sugar and alcohol and produce toxins, such as lipopolysaccharide (LPS), that can damage the gut wall, cause local inflammation and get into the bloodstream, causing inflammation in the blood vessels, contributing to atherosclerosis. These bacteria and their products can also compromise the integrity of gut wall, resulting in substances from the gut leaking into the bloodstream and undermining our health.
TMAO
Some gut bacteria also produce a substance called trimethylamine (TMA) from foods rich in L-carnitine (meat) and choline (eggs) and the liver then turns it into trimethylamine N-oxide (TMAO). TMAO is dangerous because it increases the stickiness of cholesterol particles and changes cholesterol metabolism in the liver which contributes to atherosclerosis and increases likelihood of blood clot formation.
Studies show that people with the highest levels of TMAO have a 2.5-fold higher risk of major cardiovascular event (heart attack or stroke) than people with the lowest levels.
Diet has an immense impact on gut bacteria and research revealed that a balanced vegan diet results in negligible TMAO levels and can significantly reduce TMAO in people whose levels are high. Read the research.
What you eat is one of the most important factors that can either increase or reduce your risk of heart disease. If you already have high blood pressure and cholesterol, your diet can help reverse the process or, conversely, it may accelerate atherosclerosis.
European Society of Cardiology, American Society for Preventive Cardiology, American College of Cardiology and American Heart Association all recommend a diet consisting predominantly of fruit, vegetables, pulses, nuts, seeds, plant protein, wholegrains and omega-3 fats, replacing saturated fat with polyunsaturated and monounsaturated fats, reducing dietary cholesterol intake and increasing intake of fibre-rich foods. In addition, they state that salt intake should be reduced, sugar intake minimised and trans fats are to be avoided completely.
They also warn against the consumption of red and processed meat – this advice is based on studies showing that red and processed meat increase heart disease risk because they contain saturated fat, haem iron, promote harmful gut bacteria and processed meat also contains an extra dose of toxins. Another important point they make is to avoid butter, lard, coconut and palm oil as these are all high in saturated fat. Read the research.
Plants contain a wide range of antioxidants that help to protect blood vessels from damage, tone down inflammation, decrease LDL cholesterol oxidation and can improve blood sugar control. A wholefood plant-based diet is naturally low in saturated fat, devoid of cholesterol, high in fibre and healthy carbohydrates, contains healthy unsaturated fats, natural nitrates (that help dilate blood vessels), a wealth of antioxidants and other health-protective compounds, and supports the growth of health-beneficial gut bacteria – all of these factors are the reason why it’s so beneficial for the heart. Read the research.
Studies show that people who eat balanced plant-based diets are less likely to develop heart disease and also less likely to die from it, or suffer a heart attack or a stroke compared to people who eat a diet rich in animal-based foods. Looking specifically at vegan and vegetarian diets, several major reviews found matching results – these diets are associated with lower cholesterol levels and an 18 to 55 per cent lower risk of heart disease. Read the research.
How to reduce the risk of heart disease or reverse it
Based on comprehensive research, clinical trials and latest studies described above and in our report, we bring you Viva!’s Six Steps for a Healthy Heart.