Other cancers

Summary
In the UK, one in two people born after 1960 will be diagnosed with cancer during their lifetime. Just four types of cancer (breast, prostate, lung and bowel) make up more than half of all cancers. Migrant studies show that lifestyle and diet play a much larger role than genes. After smoking, poor diet is the most important avoidable cause and people who eat meat have a higher risk.
The US NIH-AARP Diet and Health Study found people who eat the most red meat had a 20-60 per cent higher risk for oesophageal, bowel, liver and lung cancer. Those eating the most processed meat had a 16-20 per cent higher risk for bowel and lung cancer.
Vegetarians and vegans have a lower risk of cancer than meat-eaters. In the UK, vegetarians have an 11 per cent lower risk and vegans 19 per cent lower. The AHS-2 had similar results; vegetarians had an eight per cent lower risk and vegans 16 per cent lower. Vegan women had 34 per cent fewer female-specific cancers.
A study of cancer in 157 countries found high intakes of animal products linked to higher rates of cancers of the breast, kidney, pancreas, prostate and thyroid. Another study found that people eating high levels of animal (but not plant) protein are over four times more likely to die of cancer.
Chicken is not a healthy option; modern supermarket chickens contain more fat than protein, much of it saturated. High-saturated fat intake increases the risk of breast, prostate and bowel cancer as well as heart disease and diabetes while animal protein increases IGF-1 levels linked to bowel and lung cancer. Haem iron from meat generates free radicals and induces oxidative stress. Chicken also contains higher levels than red meat of the carcinogenic compound PhIP.
In 2015, the WHO announced that processed meat does cause cancer and that red meat probably does too. Just 50g of processed meat (less than two slices of bacon) a day increases the risk of bowel cancer by 18 per cent. Current guidelines need to be amended to reflect the now indisputable link between meat and cancer. Cigarettes carry government health warnings, why shouldn’t bacon and chicken nuggets?
Every year, there are more than 10 million new cases of cancer around the world; they are not spread evenly across the globe (Cross et al., 2007). In 2012, the age-standardised incidence rate (how many out of every 100,000 people will have the disease in a given year) for all cancers for men and women across the globe was 182 people per 100,000. In the UK, the figure was 273 per 100,000 (GLOBOCAN, 2012). For men, the rate varied almost seven-fold from 57 per 100,000 in Niger in Western Africa to 374 per 100,000 in Australia, where prostate cancer represents a significant proportion. Variation among women was nearly five-fold, from 70 per 100,000 in the Gambia to 328 per 100,000 in Denmark, where high rates of breast cancer occur. Denmark has been called the cancer capital as the highest cancer rate for men and women together occurs there with 338 people per 100,000 diagnosed in 2012.
| Type of cancer | Percentage of total cancers |
|---|---|
| Breast* | 15.6 |
| Prostate | 13.4 |
| Lung | 12.6 |
| Bowel | 11.5 |
| Other | 46.9 |
Table 1.0 Types of cancer registered in the UK in 2014.
Source: Office for National Statistics, 2014.
*46,085 cases in females and 332 in males.
In the UK, one in every two people born after 1960 will be diagnosed with some form of cancer during their lifetime (Ahmad et al., 2015). Although there are more than 200 different types of cancer, the four most common (breast, prostate, lung and bowel cancers) account for more than half of all cancers (NHS Choices, 2014a). Table 1.0 shows the percentages of total cancers these four most common cancers make up.
Figure 1.0 Most common cancers in England in 2013 for women and men by percentage.
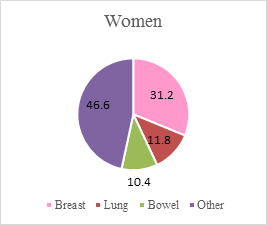
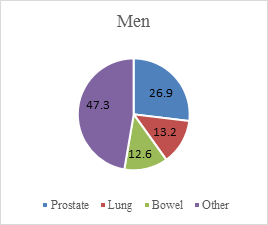
Source: Bate and Baker, 2015.
Figure 1.0 shows that three most common cancers account for over half of all cancers in women and men. Lung and bowel cancer make up nearly a quarter of cancers in both genders, while breast and prostate cancer comprise over a quarter of cancers in women and men respectively.
Smoking is the most important preventable cause of cancer; responsible for one in four UK cancer deaths and nearly a fifth of all cancer cases (Public Health England, 2016a). Nearly half of all smokers will eventually die from smoking-related diseases. After smoking, poor diet is the most important avoidable cause of cancer.
Countries with relatively high intakes of meat and other animal foods have higher rates of bowel, breast and prostate cancer (Key et al., 2014). Indeed, meat consumption has been recognised as a risk factor for cancer since the early 1900s. A study of cancer rates in different ethnic groups in Chicago from 1900-1907 found that heavy meat-eaters (Germans, Irish and Scandinavians) had higher rates of cancer mortality than pasta-consuming Italians and rice-eating Chinese (Grant, 2014).
Professor T. Colin Campbell, Jacob Gould Schurman Professor Emeritus of Nutritional Biochemistry at Cornell University in the US, is the author of over 300 research papers and co-author of The China Study (Campbell and Campbell, 2005), one of America’s best-selling books about the impact of diet on our health. His legacy, the China Project, is the most comprehensive study of health and nutrition ever conducted.
The China Project was conceived in 1980-1981 when Dr Chen Junshi (Deputy Director of the Institute of Nutrition and Food Hygiene at the Chinese Academy of Preventive Medicine) visited Campbell’s laboratory at the Division of Nutritional Sciences at Cornell University in Ithaca, New York in the US. They were later joined by Professor Richard Peto from the University of Oxford in the UK and Dr. Li Junyao from the China Cancer Institute at the Chinese Academy of Medical Sciences in China. The project demonstrated important relationships between dietary patterns and cancer risk across different countries (Campbell and Junshi, 1994). It involved 65 Chinese counties and focused on their diets and health.
Campbell and Junshi found that several major diseases including a number of different cancers as well as CVD and diabetes were all associated with affluent diets. In other words, these diseases were directly associated with the intake of meat, milk, eggs, animal fat and animal protein whilst diets high in fibre, antioxidants (mainly from fruit and vegetables) and pulses had a preventative effect.
It had previously been suggested that animal protein increases the risk of cancer. The extensive China Study found a direct link between dietary protein intake and cancer; the more protein in the diet, the higher the risk of cancer. But this did not apply to all protein, just animal protein.
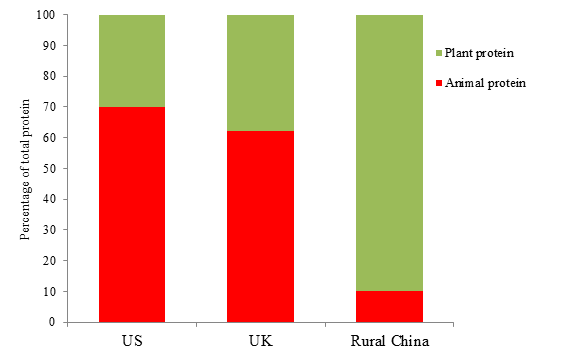
Figure 2.0 A comparison of animal protein intake in the US, UK and rural China.
Source: Campbell and Campbell, 2005; Henderson et al., 2003.
It is widely acknowledged that the incidence of certain cancers is much greater in some countries than others. What intrigued Campbell was the relationship between animal protein and these cancers. Figure 2.0 shows the differences in animal protein intake between the US, the UK and rural China. In the US, over 15 per cent of total energy intake comes from protein of which 70 per cent is animal protein (Campbell and Campbell, 2005). In the UK, over 16 per cent of food energy comes from protein and of this, 62 per cent comes from animal foods (Henderson et al., 2003). While in rural China, the figures are quite different; nine to 10 per cent of total energy comes from protein and only 10 per cent of that is from animal protein (Campbell and Campbell, 2005).
It could be argued that the difference in cancer incidence between cultures reflects genetic differences between ethnic groups rather than environmental (dietary) effects. However, migrant studies have shown that as people move from a low-cancer risk area to a high-cancer risk area, they assume an increased risk within two generations (WCRF/AICR, 2007). Therefore these vast differences in cancer rates must be largely attributable to environmental factors such as diet and lifestyle. Campbell concluded that animal-based foods are linked to an increased cancer risk whereas a wholegrain plant-based diet including fibre and antioxidants is linked to lower rates of cancer (Campbell and Campbell, 2005).
Campbell has extensively pursued, for many years, the hypothesis that dietary protein enhances tumour development. Several mechanisms have been proposed including how diets rich in animal protein (meat and dairy) drive the synthesis of the growth factor insulin-like growth factor 1 (IGF-1) in the liver, which increases the risk of a range of cancers. A 2006 a study published in the American Journal of Clinical Nutrition found that compared to a typical Western diet, a low-protein, low-calorie diet was associated with significantly lower IGF-1 levels (Fontana et al., 2006). Campbell acknowledged the importance of this finding but said in his opinion the links between animal protein and IGF-1 production are only one of these countless and highly interdependent cause and effect relations that occur in human nutrition (Campbell, 2007).
Other studies have focused directly on meat. The NIH-AARP Diet and Health Study presents information on the impact of diet and lifestyle factors on risk of cancer. In 1995-1996, nearly half a million US men and women, aged 50-71, none of whom had had cancer, joined the study. They completed a questionnaire about their dietary habits with personal information such as age, weight and smoking history. During an average of seven years follow-up, 53,396 cases of cancer were reported. This information was used to identify links between the amount of meat they ate and the incidence of various cancers (Cross et al., 2007).
Results showed that those who ate the most red meat had a 20-60 per cent higher risk for oesophageal, bowel, liver and lung cancer compared to those eating the least. Those who ate the most processed meat had a 20-16 per cent higher risk for bowel and lung cancer respectively. The authors discussed different mechanisms linking meat to cancer; saturated fat, haem iron, NOCs, HCAs and PAHs. They suggested that the link between saturated fat and cancer is likely to be related to energy balance; this means too many calories. A diet high in saturated fat, leading to obesity, increases the risk of breast, prostate and bowel cancer as well as heart disease and diabetes. The increased risk of the hormone-related cancers (breast and prostate) may result from increased levels of hormones synthesised in adipose (fat) stores in the body (Gerber and Corpet, 1999).
We know that diets rich in animal protein (meat and dairy) increase IGF-1 which increases the risk of a range of cancers, including bowel and lung cancer. Iron is also thought to contribute to an increased cancer risk by generating free radicals and inducing oxidative stress (see figure 3.0). The authors of the NIH-AARP Diet and Health Study also pointed out how exposure to NOCs occurs from eating nitrite-preserved meats as well as endogenous formation in the gut, which is directly related to the haem iron content of meat. They concluded that reducing meat intake to match the lowest intake in the study group could reduce the incidence of cancer at multiple sites. As stated previously, people in the NIH-AARP study eating 53g of red meat per day could still be classed in the lowest intake group. Avoiding meat entirely would be even more effective in preventing cancer.
A UK study from the University of Oxford, looking at how different diets affects cancer risk, revealed that people who don’t eat meat have a much lower risk of getting the disease. The 15-year study was a pooled analysis of two prospective studies including 61,647 British men and women (32,491 meat-eaters, 8,612 fish-eaters, 18,298 vegetarians and 2,246 vegans) among whom there were 4,998 cases of cancer (Key et al., 2014). Results showed that compared with meat-eaters, cancer incidence was 12 per cent lower in fish-eaters, 11 per cent lower in vegetarians and 19 per cent lower in vegans. This adds to a huge body of evidence showing how meat increases the risk of cancer and other diseases (Key et al., 2014).
The results of the US Adventist Health Study II (AHS-2) were similar, with total cancer risk significantly lower in vegetarians and vegans than in meat-eaters (Tantamango-Bartley et al., 2013). This study examined the association between diet and cancer incidence among 69,120 people among whom 2,939 cancer cases were identified during an average of four years follow-up. In this typically low-risk population, avoiding meat clearly conferred protection against cancer. Vegetarians had an eight per cent lower risk of cancer and vegans had a 16 per cent lower risk. In addition to this, vegan women experienced 34 per cent fewer female-specific cancers. The authors pointed out that the meat-eaters in AHS-2 consume much less meat than the average American. So people eating diets mainly based on meat and dairy are likely to have an even higher risk of cancer than the meat-eaters in AHS-2.
Two key studies found vegetarians have an 8-11 per cent lower risk of cancer and vegans a 16-19 per cent lower risk.
An international study comparing rates of 21 different cancers in 157 countries (reported in 87 studies in 2008), found that people who ate the most animal products had the highest rate of cancers of the breast, kidney, pancreas, prostate and thyroid (Grant, 2014). An interesting feature of this study was the time lag observed between increasing cancer rates and national dietary changes as countries adopt a more Western diet, rich in meat and dairy. Results revealed a 15-30 year lag between diet and cancer mortality; 15-27 years for bowel cancer and 20-31 years for breast cancer in Japan and 10 years for mortality rates for a number of different cancers in several Southeast Asian countries. The author said this study reiterates that animal products are an important risk factor for many types of cancer. Mechanisms discussed, linking animal products to cancer, included increased production of insulin, IGF-1 and sex hormones as well as haem iron giving rise to free radicals, oxidative stress and DNA damage. The author concluded that eating animal products is as important as smoking for increasing the incidence of all cancer types apart from lung cancer.
Even moderate intakes of animal protein are linked to a higher risk of cancer. A large cross-sectional study from the US looked at protein intake and cancer rates in 6,381 people over 18 years. Results showed those reporting a high animal protein intake had a 75 per cent higher chance of dying from all-causes during the follow-up period than people eating much less animal protein. The high-protein group were more than four times more likely to die of cancer than those in the low-protein group (Levine et al., 2014). These associations were either abolished or weakened if the source of protein was plant-based. The authors concluded that taken together, these results indicate that people aged 50-65 consuming moderate to high levels of animal protein display a major increase in their risk for cancer which could be reduced if the protein did not come from an animal source. They suggested high levels of animal protein increasing IGF-1 and possibly insulin may be responsible for the links between animal protein and cancer. These results are in agreement with recent findings on the association between meat consumption and death from all-cause, CVD and cancer (Fung et al., 2010; Pan et al., 2012).
Red and processed meat intake has long-been associated with increased risks of bowel cancer as well as several other cancers (WCRF/AICR, 2007). Several compounds either found in meat or created in it by high-temperature cooking are now known as being potential carcinogens including: NOCs, HCAs and PAHs. Haem iron and iron overload can also increase cancer risk through a range of processes including the promotion of NOC formation, increased colonic cytotoxicity and epithelial proliferation, increased oxidative stress and iron-induced hypoxia signalling (Pan et al., 2012). In other words, it contributes to compounds that can damage the cells in the colon and lead to cancer.
Chicken and PhIPs
Poultry is a source of haem iron too and is a source of potential carcinogens particularly when cooked at high temperatures. Grilling or barbecuing meat results in the formation of HCAs and PAHs, which are potent carcinogens. PhIP is the most abundant HCA detected in the human diet. The IARC has classified PhIP as possibly carcinogenic to humans. PhIP is formed at high temperatures in a reaction between substances found in meats and sugar and depends on the method of cooking and the variety of meat and increases with the temperature and duration of cooking. Research shows that high levels of PhIP have been found in chicken that was pan-fried, oven-grilled or barbecued. In these samples, PhIP levels were much higher than amounts reported previously in red meats (Sinha et al., 1995).
WHO says meat does cause cancer
Viva!Health have been warning people about the links between meat and cancer for years and in 2015, just ahead of World Vegan Day on November 1, the World Health Organisation (WHO), one of the most-respected authorities on health, published a press release stating that processed meat does cause cancer and that red meat probably does too (WHO/IARC, 2015). This was significant because the meat industry has dismissed previous claims linking meat to cancer as ‘unscientific’ or ‘simplistic’. They are still arguing the toss but even they must now realise that they have lost the argument and are clearly trying to defend the indefensible.
The International Agency for Research on Cancer (IARC) is the specialised cancer agency of the WHO. In October 2015, 22 scientists from ten countries met at the IARC in Lyon, France, to evaluate the carcinogenicity of the consumption of red and processed meat to decide if red and processed meats cause cancer. Their findings, published in The Lancet Oncology, hit the headlines around the world. They said that eating just 50 grams of processed meat (less than two slices of bacon) a day increases the risk of bowel cancer by 18 per cent.
Here are three main findings from their report:
- Overall, the Working Group classified consumption of processed meat as “carcinogenic to humans” on the basis of sufficient evidence for bowel cancer. Additionally, a positive association with the consumption of processed meat was found for stomach cancer.
- The Working Group classified consumption of red meat as “probably carcinogenic to humans”.
- In making this evaluation, the Working Group took into consideration all the relevant data, including the substantial epidemiological data showing a positive association between consumption of red meat and bowel cancer and the strong mechanistic evidence. Consumption of red meat was also positively associated with pancreatic and with prostate cancer.
Source: Bouvard et al., 2015.
Current guidelines need to be amended to reflect the now indisputable link between meat and cancer. Cigarettes carry government health warnings, why shouldn’t bacon? The government acknowledge the link between eating a lot of red meat and bowel cancer but they should now go further and warn people sufficiently about the risks associated with eating meat. Although much of the battle against cancer emphasises early detection and treatment, the burden of cancer in terms of both personal suffering and the financial strain on health services, will remain high unless the primary risk factors are understood and addressed.
Summary
Breast cancer rates continue to rise, year on year. One in eight women in the UK will now be diagnosed at some point in their lives. Rates around the world vary widely with highest levels in North America and Europe. Only five to10 per cent are caused by genes; the vast majority are caused by lifestyle and environmental factors.
As the Western diet spreads around the world, so does breast cancer. The Shanghai Breast Cancer Study found that women eating Western-style diet containing meat, fish, bread and sugary foods had a higher risk of breast cancer than those eating a traditional diet rich in vegetables and soya.
The evidence against meat is mounting. The US Nurses’ Health Study II found that women eating one-and-a-half daily servings of red meat had a 22 per cent higher risk of breast cancer than those eating one serving a week. Each additional daily serving increased the risk by 13 per cent or 54 per cent among those using oral contraceptives! Women who had eaten the most meat in adolescence had a 42 per cent higher risk of premenopausal breast cancer, but those who had eaten the most fruit had a lower risk.
Plant-based diets lower the risk of breast cancer. A study from Singapore found that over five years, diets rich in plant foods lowered the risk by 63 per cent in postmenopausal women. The Italian ORDET study found that those eating the most plant foods had a 34 per cent lower risk – it was 50 per cent lower in those with a BMI over 25.
The EPIC studies show that diets rich in fibre from vegetables lower the risk. The UK Women’s Cohort Study found that premenopausal women eating the most fibre had a 52 per cent lower risk than those eating the least.
Evidence for the harmful role of meat is as strong as that for the protective role of a low-fat, high-fibre, vegan diet consisting mainly of fruits, vegetables, wholegrains and pulses. Providing preventative dietary advice to the seven million women who attend mammography screening every three years in the UK could help reduce breast cancer incidence substantially.
Breast cancer is the most common type of cancer in the UK, with 150 women and at least one man diagnosed every day. Breast cancer incidence rate in the UK has increased by over 70 per cent since the 1970s. Just in the eight years from 1995-2003 it rose by 23 per cent (Bate and Baker, 2015). Now one in every eight women in the UK will develop breast cancer at some point in their lives.
Breast cancer rates vary greatly around the world, the age standardised rate now exceeds 100 per 100,000 in Belgium and Denmark and rates in North America, Northern and Western Europe, Australia and New Zealand are not far behind. Moderate rates are seen in South America, Southern Africa and Western Asia, but these are increasing. The lowest rates of breast cancer are found in East and Middle Africa and South-Central and East Asia.
Much is made of the link between genes and breast cancer. However, only 5-10 per cent of all breast cancers are thought to be linked to an inherited breast cancer gene (Apostolou and Fostira, 2013). This means that the vast majority of cancers (90-95 per cent) are not caused by genes. It is also important to remember that having a known breast cancer gene does not mean that a person will definitely develop the disease, it means they are more at risk of developing it.
A range of lifestyle and environmental factors can also increase breast cancer risk including: age, alcohol, obesity, high-animal/low-plant product diet, early puberty, late menopause, late age at first childbirth, hormone replacement therapy (HRT) and the contraceptive pill. Factors that may reduce the risk include: younger age at first pregnancy, high-plant/low-animal product diet, breastfeeding, late puberty, early menopause and physical activity. You can’t control all of these risk factors (age, puberty, menopause) but you can change your body weight, the amount of physical activity you do and of course your diet. These three factors have all been linked to breast cancer and are areas where you can take action.
Migration studies show us that the variation in breast cancer rates around the world is not due to genetic factors and that lifestyle factors must be involved. For example, one study found that breast cancer rates among US-born Chinese women were 80 per cent higher than among their foreign-born counterparts (Gomez et al., 2010).
In 2007, a study showing how a Western-style diet is increasing the risk of breast cancer in an Asian population was published. The Shanghai Breast Cancer Study compared the diets of 1,446 women from Shanghai recently diagnosed with breast cancer with those of 1,549 age-matched women without the disease (Cui et al., 2007). Two distinct dietary patterns were identified: ‘vegetable-soy’ (characterised by tofu, cauliflower, beans, bean sprouts and green leafy vegetables) and ‘meat-sweet’ (characterised by pork, poultry, organ meats, beef and lamb as well as shrimp, saltwater fish, and shellfish, candy, dessert, bread and cow’s milk – notably rich in saturated fats and red meat). The authors said these diets resemble the two primary patterns consistently identified across the US and Europe sometimes referred to as ‘prudent’ and Western.
Results showed the ‘meat-sweet’ diet significantly increased the risk of breast cancer in postmenopausal women, especially those who were overweight and with oestrogen receptor-positive breast cancer. These results are consistent with previous analyses of the same cohort that found that red meat, especially well-done red meat, increased breast cancer risk in premenopausal and postmenopausal women. The authors said their findings indicate that red meat intake in Shanghai occurs in a recognisably Western-influenced dietary pattern now emerging in Asian populations.
Another study, this time from Singapore, evaluated the role of diet in breast cancer (Butler et al., 2010). A large group of 34,028 women were followed for up to 12 years during which time 629 breast cancer cases recorded. Two dietary patterns were identified; the ‘meat-dim sum’ pattern and a ‘vegetable-fruit-soy’ one. Results showed that postmenopausal women eating the most plant-based foods had a 30 per cent lower risk of breast cancer. Those on the mostly plant-based diet followed for more than five years had a 63 per cent lower risk. The authors suggested possible protective roles are conferred by substances found in cruciferous vegetables (cauliflower, cabbage, bok choy, broccoli, Brussels sprouts and similar green leafy vegetables) and soya isoflavones (a phytoestrogen or natural plant hormone). So in these two studies of traditionally low-risk populations, a harmful role for a meaty diet and a protective role for a plant-based diet was observed.
Of course the protective role of a plant-based diet is not limited to any particular country. The ORDET study from Northern Italy found that women consuming higher levels of plant-based foods had a 34 per cent lower risk of breast cancer, those with a BMI over 25 had an even greater risk reduction – over 50 per cent less risk (Sieri et al., 2004). The authors concluded that a diet rich in raw vegetables and olive oil protects against breast cancer.
The US Nurses’ Health Study II provides some striking evidence; they found that women who ate one-and-a-half servings of red meat per day had a 22 per cent increased risk of breast cancer compared with women who ate one serving of red meat per week (Farvid et al., 2014). In this study, each additional serving of red meat per day was associated with a 13 per cent increase in risk of breast cancer. The authors said: “When this relatively small relative risk is applied to breast cancer, which has a high lifetime incidence, the absolute number of excess cases attributable to red meat intake would be substantial and hence a public health concern”. A further finding in this study was that for each serving per day of red meat, the risk of breast cancer was 54 per cent higher among women using oral contraceptives. The authors suggest that replacing one serving per day of red meat with pulses (peas, beans and lentils) could lower breast cancer risk by 15 per cent among all women and 19 per cent among premenopausal women.
In a subsequent study, women from the same cohort (Nurses’ Health Study II) were asked to provide information about their diets during adolescence (Farvid et al., 2015). Most breast cancer studies look at the diets of women in midlife or later. The hypothesis was that during adolescence and early adulthood mammary glands may be more susceptible to carcinogenic exposure. The authors developed this idea based on the fact that girls and young women exposed to radiation resulting from the atomic bombings of Hiroshima and Nagasaki had a higher risk of breast cancer later in life, but women exposed at age 40 or older did not have an increased risk. Results showed higher consumption of red meat during adolescence was associated with a 42 per cent increased risk of premenopausal breast cancer.
Why is red meat a potential cause of breast cancer?
“Carcinogenic by-products such as heterocyclic amines and polycyclic aromatic hydrocarbons, created during high temperature cooking of meat; animal fat and haem iron from red meat; and hormone residues of the exogenous hormones for growth stimulation in beef cattle are some of the mechanisms that may explain the positive association between high intake of red meat and risk of breast cancer” Farvid et al., 2014.
Researchers looked at fruit and vegetable intake in relation to breast cancer risk in the Nurses’ Health Study II cohort and found an association between higher fruit intake and lower risk of breast cancer (Farvid et al., 2016). For individual fruits and vegetables, greater consumption of apple, banana and grapes during adolescence and oranges and kale during early adulthood was significantly associated with a reduced risk of breast cancer.
Research from the large EPIC study also found that diets rich in fibre from vegetables were associated with a reduced risk of breast cancer (Ferrari et al., 2013). Similar results were reported by the UK Women’s Cohort Study in which 607 breast cancer cases were recorded among 35,792 women (Cade et al., 2007). The amount of fibre consumed by these women ranged from less than 20g per day to over 30g per day. Results showed that premenopausal women eating the most fibre had a 52 per cent lower risk of breast cancer than those eating the least. The authors concluded that these findings suggest that in premenopausal women, total fibre is protective against breast cancer; in particular, fibre from cereals and possibly fruit.
Another study looked at the effects of a high-fibre, low-fat diet and exercise on breast cancer risk factors including oestrogen, obesity, insulin and IGF-I in a group of overweight and obese postmenopausal women (Barnard et al., 2006). They were given a diet containing 30-40g of fibre per day and a fat intake of 10-15 per cent of total calorie intake (the government recommends our fat intake should not exceed 35 per cent of our calorie intake but the most recent NDNS found the average UK intake was 36 per cent (Bates et al., 2014). After two weeks of this diet and daily exercise classes (walking on a treadmill) the women lost weight (around 2kg) and levels of oestrogen, insulin and IGF-I were all significantly reduced.
Almost seven million women in England now regularly attend NHS mammography screening every three years. Assessing their personal breast cancer risk and providing preventative lifestyle advice could help reduce breast cancer incidence substantially. In a survey of 1,803 women, two-thirds associated lifestyle factors with breast cancer but many seemed unaware of specific risk factors such as weight gain, dietary factors, obesity, alcohol consumption and physical inactivity (Fisher et al., 2016). Attendees have already indicated their wish to have lifestyle advice at NHS breast screening clinics, but this is still not routinely provided. Such an initiative could help women be more proactive in preventing breast cancer.
Dietary advice should include how a low-fat, high-fibre, dairy-free, meat-free diet consisting mainly of fruits, vegetables, wholegrains and pulses can result in a major reduction in breast cancer risk factors.
Summary
Like breast cancer, prostate cancer rates are rising and one in eight men in the UK will get prostate cancer at some point in their lives. Rates vary widely around the world but as the Western diet spreads, so does prostate cancer.
Meat (particularly red, processed and well-done meat), is linked to a higher risk of prostate cancer. A US study found that during a week, three servings of red meat, one and a half servings of processed meat, one serving of grilled red meat or one serving of well-done red meat were each associated with a 50 per cent increased risk of advanced prostate cancer.
There is a link with poultry too, especially chicken and turkey with skin as well as hot dogs and sandwiches made with chicken and turkey. In the CaPSURE study, men eating the most poultry with skin had more than double the risk of prostate cancer progression than those eating the least. The PCRM found that diets high in saturated fat are associated with a threefold risk of cancer progression and death. Disease progression was slower in men who ate flaxseed and lycopene-containing foods like tomatoes.
The Prostate Cancer Lifestyle Trial showed that men with early-stage prostate cancer might be able to avoid or delay conventional treatment by adopting a low-fat, vegan diet. This sort of dietary advice on how a vegan diet, high in fibre and phytonutrients and low in fat and saturated fat, may prevent and slow prostate cancer, could provide men with a focus for action and a means of regaining control.
Prostate cancer is the most common cancer in men. Across the UK, over 47,000 men are diagnosed with it every year – 130 men every day. Prostate cancer incidence rates have increased by 155 per cent in men in the UK since the late 1970s. Some of this may be down to increased testing but the fact remains that in the UK, about one in eight men will get prostate cancer at some point in their lives.
Prostate cancer incidence varies more than 25-fold worldwide; the pattern is similar to that of breast cancer incidence with the highest rates seen in Australia, New Zealand, North America, Western and Northern Europe, where the age-standardised rate is around 100 men per 100,000 (GLOBOCAN, 2012). Incidence rates are also relatively high in some less affluent regions such as the Caribbean (79.8), Southern Africa (61.8) and South America (60.1), but remain low in Asian populations with estimated rates of 10.5 in Eastern Asia and 4.5 in South-Central Asia.
This leading cause of cancer death in most developed countries is now emerging as a major public health problem in developing countries too (Jemal et al., 2011). Prostate cancer incidence rates have been rapidly increasing in China, Korea, Japan and Singapore during the last few decades (Zhang et al., 2012). This increase is thought to be caused by the gradual change towards the Westernised diet with high intakes of energy, animal fat and meat and a low intake of fibre (Gathirua-Mwangi and Zhang, 2014).
Migrant studies provide further evidence that diet plays a role in prostate cancer as remarkable increases in this disease have been observed among men who move from East Asia to North America (Gathirua-Mwangi and Zhang, 2014). High consumption of meat (particularly red, processed and well-done meat), is associated with an increased risk of prostate cancer (John et al., 2011). A review of 46 studies found that saturated fat, well-done meat and calcium are all consistently linked to an increased risk for advanced prostate cancer (Gathiru-Mwang and Zhang, 2014). Interestingly, calcium from dairy products, but not calcium from other foods was associated with the risk of prostate cancer (Allen et al., 2008).
In a US study of men from the Greater San Francisco Bay Area, weekly consumption of three or more servings of red meat, one and a half or more servings of processed meat, one or more serving of grilled red meat and one or more serving of well-done red meat were each associated with a 50 per cent increased risk of developing advanced prostate cancer (John et al., 2011).
In this study of men from the Greater San Francisco Bay Area, although the increased prostate cancer risk was associated with grilled and well-done red meat, they found no consistent associations with HCAs (except for a possible link with advanced disease and PhIP). However, more than 15 different HCAs are known to accumulate in cooked meat, yet usually only three (PhIP, MeIQx and DiMeIQx) are measured and compounds formed at lower concentrations, which are not measured or not-yet identified, may play a role in prostate cancer (Joshi et al., 2012). While this study also found no consistent association with BaP (the most abundant PAH) the authors said that they couldn’t exclude the possibility that other PAHs formed during cooking may underlie the link between grilled red meat and prostate cancer.
Another study, looking at 2,770 cases of prostate cancer among 26,030 men did find a positive association between PhIP from red meat and prostate cancer, particularly high-grade (fast-growing) and possibly also advanced prostate cancer (Rohrmann et al., 2015). However, they noted that while PhIP intake from red but not from white meat was linked with prostate cancer, PhIP intake from white meat is twice as high as that from red meat. This, they said, argues against PhIP (or HCAs in general) as the factor responsible for the link between meat and prostate cancer and suggests that some other mutagenic compounds arising from meat may be the causal factor. More research is required to fully-elucidate the underlying mechanisms.
The research on how diet may affect progression of prostate cancer after diagnosis is of great interest given the large numbers of men diagnosed with this disease. Researchers from the Physicians Committee for Responsible Medicine (PCRM) reviewed eight observational studies and 17 intervention studies on the effect of diet on prostate cancer and found that diets high in saturated fat are associated with a threefold higher risk of cancer progression and death, compared with a diet low in saturated fat (Berkow et al., 2007). This review revealed a slowing of disease progression in prostate cancer patients consuming flaxseed and lycopene-containing foods (tomatoes are a rich source of lycopene). The authors concluded that plant-based diets – high in fibre and phytonutrients and low in fat and saturated fat – favourably influence health outcomes for prostate cancer patients.
Another study looking at how diet may affect disease progression found that two and a half eggs per week increased the risk of lethal prostate cancer by 81 per cent compared to less than half an egg per week (Richman et al., 2011). They also found a link between poultry and processed meat and progression to lethal prostate cancer, but these associations were of borderline statistical significance. The association with poultry appeared to be driven by poultry and poultry products with skin (chicken or turkey with skin, chicken or turkey hot dogs and chicken or turkey sandwiches). The authors said they had limited power to examine individual poultry items due to low consumption of these foods in their study population. Those eating three and a half servings a week of poultry products were put in the highest consumer group; many people eat a lot more chicken than that. Also, the men who ate the most poultry in this study engaged in more vigorous activity, were less likely to be smokers and consumed less red meat, dairy and coffee than men who ate the least poultry. These factors may have contributed somewhat to masking the harmful effects of poultry in this relatively healthier-living group of low-consumers.
The relationship between eating poultry with skin after diagnosis and clinical outcomes (or disease progression) in men with prostate cancer has been examined before. In the CaPSURE study, men who ate the most poultry with skin had more than double the risk of prostate cancer progression compared with men who ate the least (Richman et al., 2010).
The Prostate Cancer Lifestyle Trial was a one-year randomised controlled clinical trial of 93 patients with early-stage prostate cancer who had chosen not to undergo conventional treatment (Ornish et al., 2005). This was a unique opportunity to observe the effects of diet and lifestyle changes without the confounding effects of radiation or surgery. The patients in the experimental group followed a vegan diet consisting of fruits, vegetables, wholegrains and pulses including soya. They also exercised, practised stress management and attended group support sessions. The control patients received the usual care. After one year, none of the vegan group had required conventional treatment but six control patients had because their disease had progressed. Prostate-specific antigen (PSA) fell four per cent in the vegan group but went up six per cent in the control group. Although the size of these changes was modest, the direction of change is important as an increase in PSA indicates disease progression. In a second test, prostate cancer cells in vitro were exposed to blood serum from both groups to see if it stimulated or decreased prostate cancer cell growth. Serum from the vegan group inhibited growth almost eight times more than serum from the control group (70 versus nine per cent), suggesting that comprehensive lifestyle changes could affect tumour growth.
In a subsequent study, after two years, just two (five per cent) of the 43 vegan patients had undergone conventional treatment but 13 (almost a third) of the 49 control patients had. Dr Dean Ornish, clinical professor of medicine and founder and president of the Preventive Medicine Research Institute, concluded that patients with early-stage prostate cancer might be able to avoid or delay conventional treatment for at least two years by making changes in their diet and lifestyle (Frattaroli et al., 2008).
Taken together, this research provides further evidence that poultry, red and processed meat are associated with increased risk of prostate cancer. While the exact mechanism underlying the links between meat and prostate cancer remain unclear, the association remains firmly established. Research shows that if health professionals can offer qualified, general advice about diet, this may provide men with a focus for action and a means of regaining control (Kassianos et al., 2015).
The links between meat and cancer explained
Several explanations have been suggested for the link between red meat and prostate cancer. HCAs formed when meat is cooked at high temperatures may account for the link between poultry after diagnosis and risk of lethal prostate cancer (Richman et al., 2010). HCAs form DNA adducts (this is when DNA becomes bound to a cancer-causing chemical) and so increase the occurrence of numerous cancers including prostate cancer (Richman et al., 2011). Chicken is a primary source of HCAs in the typical Western diet and fried, roast and grilled chicken can contain particularly high amounts of HCAs.
Another obvious culprit is the saturated fat in meat, which has long been proposed as a risk factor. Total and saturated fat intake have both been positively associated with PSA levels (this is a protein produced by the prostate gland used to assess disease progression), increased risk of prostate cancer and aggressive prostate cancer, while saturated fat intake has been associated with fatal prostate cancer (Bishop et al., 2015).
However, results of some studies of dietary fat and prostate cancer are inconsistent, some having a link with red meat but not fat. Other explanations include the presence of haem iron in red meat, which may catalyse oxidative reactions. Finally, an association between prostate cancer and meat intake may be due to potent chemical carcinogens generated during cooking and processing of red meat and poultry, such as NOCs, HCAs and PAHs. The prostate gland is able to metabolise these chemicals into activated carcinogens (Joshi et al., 2012).
The telomere study
In a later study, Ornish focussed on telomeres, stretches of DNA that protect the ends of our chromosomes rather like the plastic caps that prevent shoelaces from unravelling (Ornish et al., 2013). Every time a cell divides, telomeres become shorter. Once they reach a critically short length, the cell stops dividing and dies. As more body cells are lost, signs of ageing begin to appear, which may be followed by age-related diseases such as cancer, stroke, heart disease, vascular dementia, obesity, osteoporosis and diabetes.
Dr Ornish worked alongside Elizabeth Blackburn, who won the 2009 Nobel Prize in Physiology or Medicine for her discovery of telomerase, the enzyme that replenishes telomeres. In this study, as before, one group followed Ornish’s lifestyle changes, the other group carried on as usual. They measured telomere length at the beginning of their study and again after five years. Among the men with low-risk prostate cancer who made comprehensive lifestyle changes (vegan diet, exercise, stress management and support group), telomere length increased significantly by an average of 10 per cent. Telomere length decreased by an average of three per cent in the control group.
This study suggests yet another possible mechanism by which lifestyle changes, avoiding meat and dairy, might help combat prostate cancer and other age-related diseases. Ornish said: “The implications of this relatively small pilot study may go beyond men with prostate cancer. If validated by large-scale randomised controlled trials, these comprehensive lifestyle changes may significantly reduce the risk of a wide variety of diseases and premature mortality”.
Despite all this evidence, advice from the NHS on the links between diet and prostate cancer remains sparse.
The data linking the consumption of poultry, red and processed meat to prostate cancer provides a convincing argument for eliminating meat (and all animal foods) from the diet while increasing the intake of wholegrain foods, pulses (including soya), fruit and vegetables, nuts and seeds.
Summary
Lung cancer is responsible for nearly one in five cancer deaths. Smoking may cause around 85 per cent of cases but evidence shows that dietary factors also influence the risk. In 2007, the WCRF said red and processed meat were a possible cause. Since then, the evidence has grown stronger.
The NIH-AARP Diet and Health Study found that those eating the most processed meat had a higher risk of lung and bowel cancer and those eating the most red meat had a higher risk of lung, bowel, liver and oesophageal cancer. Men eating the most red meat had a 22 per cent higher risk of lung cancer and women eating the most, a 13 per cent higher risk. Processed meat increased the risk for men by 23 per cent. High intakes of haem iron and low intakes of antioxidants increased the risk even more.
Studies from Uruguay, Europe, Asia, the US, Canada and Australia found that that red and processed meat increase the risk of lung cancer. Each additional 120g of red meat a day increased the risk by 35 per cent while an additional 50g of red meat increased it by 20 per cent. Another study found that a high intake of red meat increased the risk by 35 per cent.
Some studies have found higher levels of the growth hormone IGF-1 in people with lung cancer. Animal protein triggers IGF-1 production in the liver and studies show vegans have lower levels than meat-eaters and vegetarians.
So meat increases the risk of lung cancer and vegetables, fruit and soya reduce it. One in ten lung (and bowel) cancers could be avoided if people reduced their red and processed meat intake. Avoiding meat altogether would be even more effective. Although stopping smoking is the most effective way to lower lung cancer risk, healthy eating could help prevent it, especially in former and current smokers.
Lung cancer is one of the most common and serious types of cancer, making up around 13 per cent of all cancers and responsible for nearly one in five cancer deaths worldwide (GLOBOCAN, 2012). Men are more likely to develop lung cancer than women, probably because they tend to smoke more. It is the most common cancer in men worldwide with the highest rates in Central and Eastern Europe (53.5 per 100,000) and Eastern Asia (50.4 per 100,000). Low rates for men are seen in Middle and Western Africa (2.0 and 1.7 per 100,000 respectively).
In women, the incidence rates are generally lower and the geographical pattern is a little different, reflecting different historical patterns of smoking. The highest rates for women are seen in North America (33.8) and Northern Europe (23.7) with a relatively high rate in Eastern Asia (19.2) and the lowest rates again in Western and Middle Africa (1.1 and 0.8 respectively).
In the UK, lung cancer incidence peaked in the 1960s, remained high until the mid-1980s, and is now declining (WCRF/AICR, 2007). Around 44,500 people are now diagnosed with lung cancer every year in the UK (NHS Choices, 2015b). Smoking is a well-established risk factor for lung cancer and is thought to be linked to 85 per cent of cases. This is because smoking involves regularly inhaling a number of different toxic substances. However, evidence suggests some dietary factors also influence the risk of lung cancer.
In 2007, red and processed meats were classified by the WCRF/AICR as possible causes of lung cancer (WCRF/AICR, 2007). When their report was published the evidence was somewhat inconsistent, but more recent studies now provide stronger evidence linking diet and lung cancer.
The huge NIH-AARP Diet and Health Study (published the same year but not included in the WCRF/AIRC report) looked at around 500,000 people aged 50-71 and found that those who ate the most red meat had an increased risk of developing lung, bowel, liver and oesophageal cancer compared with those who ate the least. Those eating the most processed meat had an increased risk of developing lung and bowel cancer (Cross et al., 2007). The authors said that one in ten lung and bowel cancers could be avoided if people reduced their red and processed meat intake. Avoiding meat altogether would certainly be even more effective.
A review of 33 studies from Uruguay, Europe, Asia, the US, Canada and Australia found that that both red and processed meat consumption increased the risk of lung cancer (Xue et al., 2014). For every additional 120g of red meat per day, the risk of lung cancer increased 35 per cent and for every additional 50g of processed meat per day, the risk increased 20 per cent.
Another review investigating the relationship between meat and lung cancer looked at 34 studies and also found that a high intake of red meat increased the risk of lung cancer by
35 per cent (Yang et al., 2012). They suggested that high levels of saturated fat present in meat may also be associated with the increased risk of lung cancer and said that more studies on meat mutagens, haem iron, meat cooking preferences and doneness level (how well done the meat is) are needed to fully characterise the meat-lung cancer association.
In a study of 242 Iranian men with lung cancer, it was found that refined grains, beef, liver, dairy products, vegetable ghee and animal ghee increased the risk, while fruit, vegetables and sunflower oil were protective (Hosseini et al., 2014). Specifically, sheep and beef livers were found to be a risk factor for lung cancer. The authors said that sheep and beef livers contain heavy metals and other poisons, as it is the organ responsible for metabolising and detoxifying food, antibiotics, vaccine ingredients, pesticide over-spray, tainted water and the synthetic hormones that are frequently given to farmed animals and this may influence cancer risk.
Not all studies have identified the link between meat and lung cancer. The Prostate, Lung, Colorectal and Ovarian Cancer Screening Trial (PLCO) recorded 782 cases of lung cancer over eight years among 99,579 people aged 55-74 years. They found no significant links between red and processed meat and lung cancer (Tasevska et al., 2011). The authors noted that the people enrolled in the PLCO trial were better educated, more physically active, more likely to be married, less likely to smoke and had lower mortality than the general population. It was assumed that they had healthier diets too and the relatively low intake of high temperature cooked meats may have affected this study’s ability to detect an association. On average, only 20 per cent of meat consumed in this cohort was cooked at a high temperature. The authors also said the relatively low follow-up period of just eight years was short compared to other studies and may have contributed to them failing to find the links others have.
Potential mechanisms linking meat consumption to lung cancer involve carcinogenic NOCs and haem iron. NOCs are found in nitrite-preserved meat and are also generated by stomach and gut bacteria from nitrites in meat. This endogenous production of NOCs is driven by haem iron also found in meat. Iron overload can activate oxidative responsive transcription factors, pro-inflammatory cytokines and iron-induced hypoxia signalling – a classical feature of cancer (WCRF/IARC, 2007).
Cooking red meat at high temperatures results in the production of HCAs and PAHs which are potent lung carcinogens. The NIH-AARP Diet and Health Study investigated the effects of red and processed meat, HCAs, BaP (the most abundant PAH) and haem iron in almost half a million people followed over eight years (Tasevska et al., 2009). Results showed a significant association between meat and lung cancer. Men who ate the most red meat had a 22 per cent higher risk of lung cancer and women who ate the most, a 13 per cent higher risk than those who ate the least. Processed meat increased the risk for men by 23 per cent. They found an even higher risk of lung cancer in men with a high intake of haem iron and lower intakes of antioxidants. The authors suggested that an unhealthy diet may disrupt the balance between pro-oxidants and antioxidants in the lung tissue and trigger oxidative damage and carcinogenesis.
High haem iron intake is associated with an increased risk of cancer of the bowel, pancreas and lung (Hooda et al., 2014). Molecular studies have revealed how haem iron may increase cancer progression. Oxygen consumption and haem synthesis are intensified significantly in lung cancer cells compared to normal cells. Thus the increase in haem availability in cancer cells and tumours leads to elevated production of haemoproteins, higher oxygen consumption and cellular energy production which fuels cancer cell progression.
Studies have shown that IGF-1 can stimulate abnormal cell growth and division and some studies have found levels are raised in people with lung cancer (Cross et al., 2007). Animal protein (meat and dairy) increases the production of IGF-1 in the liver and vegans, who don’t eat animal protein, have been found to have lower levels of IGF-1 circulating in the blood. One study found that the average IGF-I concentration was 13 per cent lower in 92 vegan women compared with 99 meat-eaters and 101 vegetarians (Allen et al., 2002), while another study found IGF-1 was nine per cent lower in 233 vegan men than in 226 meat-eaters and 237 vegetarians (Allen et al., 2000).
A review of eight studies, with 13,548 lung cancer cases among 108,748 people, found that a healthy diet lowered lung cancer risk (Sun et al., 2016). They found that high intakes of vegetables, fruit and soya reduced risk, while red meat and processed meat increased risk. The authors said that the mechanism here is undoubtedly related to anti-tumourigenic (anti-tumour-forming) agents found in the individual components of a healthy plant-based diet, including antioxidants, polyphenols, fibre and minerals. Thus, although stopping smoking is still the most effective approach to lowering lung cancer risk, healthy eating and lifestyle are also necessary for the prevention of lung cancer, especially for former and current smokers.
“The evidence that fruits protect against lung cancer is convincing” (WCRF/IARC, 2007).
Summary
Bowel cancer is one of the most common types of cancer in the UK affecting about one in every 20 people. Wide geographical variation indicates a role for diet and lifestyle factors. High intakes of meat are consistently linked with a higher risk, which is why the WCRF recommend that people limit their intake of red meat and avoid all processed meat.
A review of 19 studies from the US, Europe, Australia and Japan found that those eating the most red meat had a 28 per cent higher risk and those eating the most processed meat, 20 per cent higher. A Canadian study found that people eating the most meat were 84 per cent more likely to have bowel cancer. Those eating the most plant-based foods were 45 per cent less likely to have the disease.
Including fibre in a meaty diet is not the answer. A study comparing the diets of African Americans and Native Africans and found that surprisingly, their fibre intake was the same, but African Americans ate more protein, fat, meat, saturated fat and cholesterol, suggesting the higher bowel cancer rate in African Americans is linked to their high intake of animal foods.
Meat consumption plays a strong role in bowel cancer risk. This may be because meat-eaters are more likely to be overweight or obese. It may be the fat, saturated fat, animal protein or the NOCs, HCAs and PAHs in meat. It may not be possible to work out which of these is doing the damage, but does it matter? A diet rich in one usually contains the others.
Bowel cancer is the leading cause of cancer death among non-smokers in developed countries. Its prevention should be a major public health concern. Given what we now know about the harmful effects of meat, isn’t it high time the government amended their health guidelines to properly reflect the risks associated with meat? Meat-eaters need the same level of health advice as smokers but are not being warned sufficiently.
Bowel cancer (also called colorectal cancer) is a general term for cancer that includes colon and rectal cancer. There is wide geographical variation in incidence across the world. The highest rates are seen in Australia, New Zealand, Europe and North America and the lowest in parts of Africa, (South Central) Asia and Central America (GLOBOCAN, 2012). In The China Study, Professor T. Colin Campbell noted that while North America, Europe, Australia and wealthier Asian countries (such as Japan and Singapore) had relatively high rates, Africa, Asia and most of Central and South America had much lower rates. Campbell noted that the Czech Republic had a death rate of 34.19 per 100,000 males, while in Bangladesh the figure was less than one (just 0.63) per 100,000 males (Campbell and Campbell, 2005).
Bowel cancer is one of the most common types of cancer in the UK, with around 40,000 new cases diagnosed every year. About one in every 20 people in the UK will develop bowel cancer in their lifetime. The varied distribution of this disease suggests that bowel cancer may be linked to diet and lifestyle choices.
The incidence of bowel cancer is much higher in African Americans than in Native Africans (60 per 100,000 versus less than one per 100,000). To explore this further, researchers compared the diets of randomly selected people from both populations and found that surprisingly their fibre intake was the same but that African Americans consumed more protein, fat, meat, saturated fat and cholesterol (O’Keefe et al., 2007). The authors concluded that the higher bowel cancer rate in African Americans is associated with their higher intake of animal products.
High intakes of red and processed meat are consistently associated with an increased risk of bowel cancer. A 2006 review of 19 prospective studies involving almost 8,000 cases of bowel cancer found that those who ate the most red meat and processed meat had a 28 per cent and 20 per cent higher risk of the disease respectively compared with those who ate the least (Larsson and Wolk, 2006). It is because of the links with bowel cancer that in its 2007 report, the WCRF recommended that people should limit their intake of red meat and avoid processed meat (WCRF/AICR, 2007).
Several theories have been put forward to explain how meat increases bowel cancer risk:
- High-fat or high-protein diets can promote carcinogenesis (the initiation of cancer)
- Potentially carcinogenic NOCs are formed in food and/or endogenously by nitrosation of amines and amides
- Cooking meat at high temperature forms mutagenic and carcinogenic HCAs and PAHs
- Haem iron in red meat can promote carcinogenesis through oxidation and DNA damage
Source: Santarelli et al., 2008.
How meat increases the risk of bowel cancer
Fat intake is a major factor that could explain the link between bowel cancer and meat. Epidemiologic studies suggest that a high intake of dietary fat promotes bowel cancer by increasing the secretion of bile acids which can promote tumours. High-fat diets are also high-calorie diets and the balance between energy intake and physical activity is still considered a major risk factor (Santarelli et al., 2008).
HCAs and PAHs are formed during the cooking of meat. As stated, various HCAs are formed according to the type of meat and method of cooking. Processed pork meat (ham and bacon) may not contain as many HCAs as pan-fried beef and chicken, but then processed meats like these contain nitrites which give rise to NOCs. The most abundant HCAs in meat are MeIQx, DiMeIQx and PhIP.
PAHs are produced from the incomplete combustion of organic compounds. Many PAHs, like BaP are mutagens and carcinogens. The main sources of PAHs for people are cooked and smoked meat and fish (notably barbecued meat) and tobacco smoke (Santarelli et al., 2008). Studies suggests that cooking methods and how well-cooked meat is, are related to bowel cancer risk; the higher the temperature, the higher the risk. A Swedish case-control study showed that frequent consumption of fried meat with a heavily browned surface led to a three-fold increase in bowel cancer risk (Gerhardsson-DeVerdier et al., 1991). In summary, HCAs and PAHs are present in the daily diet of meat-eaters; they are proven carcinogens and can lead to bowel cancer.
Another mechanism underlying the links between meat consumption and cancer, is the generation by gut bacteria of carcinogenic NOCs (WCRF/AICR, 2007). NOCs are found preformed in a range of foods including nitrite-preserved processed meats (hot dogs contain 10 times more NOCs than fresh red meat), smoked fish and cheeses (Santarelli et al., 2008). However, the amount of NOCs in human faeces can exceed the amount in the diet by more than 10-fold suggesting endogenous formation in the gut (Holtrop et al., 2012). One study found NOCs in the faeces were 30-fold greater than levels in the diet (Hughes et al., 2001). Another study found the faecal concentration of NOCs was 60 times higher in volunteers given cured red meat than in volunteers given a vegetarian diet (Joosen et al., 2009).
Endogenous production is likely to begin with the formation of nitrosothiols (organic compounds containing a nitroso group) in the stomach, as acidic conditions favour the formation of these compounds (Kuhnle et al., 2007). The gastrointestinal tract then provides favourable conditions for the formation of NOCs. Haem iron stimulates the production of NOCs in the intestines (Cross et al., 2012). In fact, haem from meat strikingly increases NOC formation (Santarelli et al., 2008).
The catalytic effects of haem iron can be inhibited by trapping it with either calcium or chlorophyll from green leafy vegetables and NOC formation can also be inhibited by vitamins C and E. Polyphenols (found in fruit, vegetables, cereals, pulses, tea and wine) can inhibit lipid peroxidation caused by free radicals, the production of which is also catalysed by nitrite-preserved meat and haem (Bastide et al., 2011). The science points to colourful fruit and green leafy vegetables offering protective benefits while all meat has to offer is a range of hidden nasties lurking within it.
Two more studies looking at whether processed meat increases bowel cancer risk by stimulating the production of NOCs, revealed the harmful effects of meat (Joosen et al., 2009). A red meat (beef and pork) diet was compared to a vegetarian diet and then a preserved meat (nitrite-preserved bacon, ham, luncheon meat and corned beef) diet was compared to a vegetarian diet. Faecal homogenates (imagine putting some poo in a blender!) were analysed for haem iron, NOC and genotoxicity. Similar to previous studies, results showed faecal NOC levels were low (3-4 nmol/g) on diets containing no meat. On preserved and red meat diets containing similar amounts of haem iron, faecal NOC levels increased substantially (to around 180 nmol/g). Results also showed that while nitrite-preserved meats have a similar effect as red meat on NOC production, processed meat caused additional DNA damage providing a possible explanation for the increased risk of bowel cancer associated with bacon, sausages, ham and other processed meats.
At the higher levels of meat consumption, concentrations of NOCs are of the same order of magnitude as the concentration of tobacco-specific NOC in cigarette smoke (Bingham et al., 2002). One study found that on a high-meat diet of 420g per day, exposure to NOC was comparable with other sources of NOC, such as tobacco smoke (Hughes et al., 2001).
So it turns out that big meat-eaters may be in need of the same level of health advice as smokers! Which is what Labour Member of Parliament for Bristol East, Kerry McCarthy suggested in 2015 in an interview for Viva!life magazine: “I really believe that meat should be treated in exactly the same way as tobacco with public campaigns to stop people eating it” (McCarthy, 2015).
According to the International Agency for Research on Cancer (IARC), the specialised cancer agency of the WHO: “Ingested nitrate or nitrite under conditions that result in endogenous nitrosation is probably carcinogenic to humans” (WHO/IARC, 2010). So bacon does cause cancer…
As many studies point out, an additional harmful effect of a diet rich in animal products is that the foods that help protect against bowel cancer (fruit, vegetables, wholegrains and pulses – rich in fibre) are excluded or replaced with meat and dairy. A Canadian study looked at three different dietary patterns among 1,000 people, half of whom had been diagnosed with bowel cancer, to determine each diet’s effect on the risk of the disease (Chen et al., 2015). The meaty-diet pattern was characterised by high amounts of red meat, processed meat, fish and processed fish. The plant-based diet featured fruit, vegetables and wholegrains. A third pattern was named sugary-diet as it consisted largely of pies, tarts, desserts and sweets. Results showed that the plant-based diet conferred a protective effect against bowel cancer, while the meat-diet pattern and the sugary-diet pattern were associated with a greater risk. Those eating the most meat were 84 per cent more likely to have bowel cancer than those eating the least, whereas those eating the most plant-based foods were 45 per cent less likely to have bowel cancer than those eating the least. The sugary pie and biscuit diet fared badly, pushing the risk up to 126 per cent!
In summary, a high consumption of meat, dairy, processed foods, chips, cakes and biscuits, characteristic of the typical Western diet, plays a strong role in bowel cancer risk. The causal mechanism may involve being overweight or obese, which previous studies have found to be important risk factors for bowel cancer (Chen et al., 2015). Other causes are fat, saturated fat, animal protein, NOCs, HCAs and PAHs. It’s not always possible to discern which component is doing the damage. Does it matter? A diet rich in one usually contains the others. Bowel cancer is the leading cause of cancer death among non-smokers in affluent countries and its prevention should be a major goal for public health. Given what we now know about the harmful effects of meat and bowel cancer, isn’t it about time the government amended health guidelines to properly reflect the risks associated with meat?
Summary
Kidney cancer is the eighth most common cancer in adults in the UK. Renal cell carcinoma accounts for more than 80 per cent of all kidney cancers.
The NIH-AARP Diet and Health Study found that those eating the most red meat had a 19 per cent increased risk compared to those eating the least. The mutagenic cooking compounds found in meat cooked at high temperatures are thought to increase the risk. BaP (a PAH marker) and PhiP (the most abundant HCA) increase the risk by 20-30 per cent. For every extra 10g of red meat, the risk increases by 13 per cent.
A Texan study found a 54 per cent increased risk associated with PhIP and a nearly two-fold increase associated with another HCA called MeIQx. Furthermore, HCAs may alter the behaviour of certain enzymes in the kidney (and liver) in such a way that they react with DNA and cause mutations which can lead to cancer.
Taken together, meat spells trouble for kidney cancer.
Kidney cancer is the eighth most common cancer in adults in the UK, with just over 10,100 people diagnosed each year (NHS Choices, 2014b). Renal cell carcinoma (RCC) is kidney cancer that starts in the lining of the proximal convoluted tubule – the small tubes in the kidney that transport waste molecules from the blood into the urine. RCC accounts for more than 80 per cent of all kidney cancers. In 2007, the WCRF/AICR report deemed the evidence for meat intake and RCC risk to be inconclusive (WCRF/AICR, 2007). Since then, a number of studies have found that mutagens from meat-cooking are associated with RCC risk.
The large NIH-AARP Diet and Health Study cohort of 492,186 people were used to investigate the link between meat-related compounds and the risk of RCC (Daniel et al., 2012). During nine years of follow-up, 1,814 cases of RCC were diagnosed. Results showed that those eating the most (62.7g per 1,000 calories) red meat had a 19 per cent increased risk of RCC compared to those eating the least (9.8g per 1,000 calories). For every additional 10g of red meat (per 1,000 kcal), the risk increased by 13 per cent. BaP (used as a PAH marker, indicating the presence of other PAHs) and PhiP (the most abundant HCA) increased the risk by 20-30 per cent. The authors concluded that it seems plausible that epithelial cells in the renal tubule would be sensitive to metabolic stress from haem iron and other dietary carcinogens related to meat intake.
Another study, among residents of Texas in the US, examined associations between the meat-cooking mutagens MeIQx and PhiP and the risk of kidney cancer in 659 newly diagnosed cases of RCC and 699 controls (Melkonian et al., 2016). In this case-control study, they observed a nearly two-fold increase in RCC risk associated with MeIQx and a 54 per cent increased risk associated with PhIP. The authors said this suggests that the intake of meat cooked at high temperatures may impact the risk of RCC through mechanisms related to mutagenic cooking compounds.
How meat might cause kidney cancer
Several research groups are now working on identifying the precise mechanism linking meat to kidney cancer. There is a group of enzymes (UDP-glucuronosyltransferases or UGTs) that perform a process called detoxification in the liver and kidneys. However, certain HCAs (AaC and PhiP) can cause the bioactivation of these enzymes, which means activating them in such a way that they can react to DNA and cause mutations which may lead to cancer. The theory is that this enzyme system, working in the kidney (and liver) to clear drugs, hormones, fats and other compounds, can contribute to the genotoxic effects of HCAs by catalysing the production of reactive compounds that bind to DNA (Cai et al., 2016).
Summary
Pancreatic cancer is the fourth most common cause of cancer death. Large geographical variation indicates diet and lifestyle as contributing to the risk of this disease.
Many studies show that meat increases the risk. The NIH-AARP Diet and Health Study found that men eating the most grilled and barbecued meat had a 50 per cent increased risk. Men and women consuming the most DiMeIQx had a 29 per cent increased risk. Another NIH-AARP study found links with fat, particularly from red meat and dairy foods but not from plant foods.
Studies from the US, Europe and Japan found that each daily 50g serving of processed meat increased the risk in men by 19 per cent. Men tend to eat more meat but it could be that haem iron was involved and women gained protection by losing iron through menstruation.
The EPIC-Oxford and the Oxford Vegetarian Study found that vegetarians and vegans were 50 per cent less likely to die from pancreatic cancer than meat-eaters. Another study of British vegetarians found the risk of pancreatic cancer was 27 per cent lower than in meat-eaters.
Another EPIC study found that for every 50g increase in poultry a day (three chicken nuggets or a third of a chicken breast) the risk of pancreatic cancer increased by 72 per cent. The same team found similar results for lymphomas and suggest drugs and antibiotics given to poultry to enhance growth and to treat disease may be involved.
These findings provide strong evidence that animal fat and meat play a role in the development of pancreatic cancer.
Pancreatic cancer is the fourth most common cause of cancer death worldwide with large geographical variation, which implies diet and lifestyle as contributors as risk factors for this disease (Rohrmann et al., 2013). Around 8,800 people are diagnosed with pancreatic cancer in the UK each year (NHS Choices, 2014c).
Meat intake has been positively associated with pancreatic cancer in many studies. The NIH-AARP Diet and Health Study cohort of 537,302 individuals, aged 50-71, investigated the association between meat, cooking methods, meat-mutagen intake and pancreatic cancer (Stolzenberg-Solomon et al., 2007). During five years of follow-up, 836 pancreatic cancer cases were recorded. Results showed that men consuming the most grilled and barbecued meat had a 50 per cent increased risk of pancreatic cancer. Men and women consuming the most DiMeIQx (an HCA found abundantly in well-cooked meat) had a 29 per cent increased risk. These findings indicate that meat, particularly meat cooked at high temperatures, plays a role in the development of pancreatic cancer.
A review of eleven studies, six from the US, four from Europe and one from Japan, found that each 50g per day (about one serving) of processed meat was associated with a 19 per cent increased risk of pancreatic cancer (Larsson and Wolk, 2012).
Few studies have examined associations between dietary fat and pancreatic cancer and their findings have been inconsistent. This may be due to the small number of patients diagnosed with pancreatic cancer and/or to the narrow range of fat intakes in these studies. The NIH-AARP study included a large number of people and wide range of fat intake from diverse food sources. This study observed significant links between pancreatic cancer and animal fat, particularly from red meat and dairy foods but did not observe any consistent association with fat from plant foods (Thiébaut et al., 2009). They concluded that animal fat is associated with an increased risk of pancreatic cancer.
How meat might cause pancreatic cancer
In the review of 11 studies from the US, Europe and Japan, the link between pancreatic cancer and red meat was only observed in men. The authors said that red meat consumption was on average higher in men than in women and suggested that if there is a threshold effect with an increased risk of pancreatic cancer only at high levels of red meat consumption, a positive association may be more likely to be detected in men. Another biologically plausible explanation for the observed differences between men and women is haem iron (abundant in red meat), which could enhance the growth of pancreatic cancer tumours (Stolzenberg-Solomon et al., 2007). Due to normal iron loss during menstruation, women do not accumulate such high iron stores as men. Higher levels of iron in the blood and higher percentage of iron saturation (iron to iron binding capacity) were associated with increased risk of subsequent pancreatic cancer in one prospective study (Friedman and van den Eeden, 1997).
Combined data from the EPIC-Oxford cohort and the Oxford Vegetarian Study (including 31,470 meat-eaters, 8,516 fish-eaters, 18,096 vegetarians and 2,228 vegans) found that, compared with meat-eaters, vegetarians and vegans had around 50 per cent lower mortality from pancreatic cancer (Appleby et al., 2016). When they excluded those who changed diet group during the study (possibly reflecting the onset of illness), compared with regular meat-eaters, vegetarians and vegans had around 50-60 per cent lower mortality. This reflects findings from another study of cancer in British vegetarians (Key et al., 2014). They found the risk of cancer is generally lower in vegetarians and vegans than meat-eaters, specifically 27 per cent lower for pancreatic cancer.
A link with poultry was found in the huge EPIC study looking at the links between meat and fish with pancreatic cancer (Rohrmann et al., 2013a). During the study, 865 pancreatic cancer cases were recorded among 477,202 participants from 10 European countries. The consumption of red and processed meat was not associated with pancreatic cancer in this study. However, for every 50g of poultry per day (that’s just three chicken nuggets or a third of a chicken breast) the risk of pancreatic cancer increased by 72 per cent.
When the same EPIC team found a similar result for lymphomas and poultry they suggested antibiotics and/or coccidiostats (drugs given to poultry or cattle to prevent the growth and reproduction of certain parasites) may be involved (Rohrmann et al., 2011). Chicken and turkeys are often treated with coccidiostats and antibiotics to enhance their growth and to treat and prevent disease. The frequency of antibiotic use has been associated with the risk of non-Hodkin lymphoma in some studies (Chang et al., 2005; Kato et al., 2003).
The EPIC team also suggest another possibility, oncogenic animal viruses. Poultry may contain viruses that cause the development of tumours, especially if the meat is not cooked properly. Oncogenic animal viruses have been suspected as a cause of non-Hodgkin lymphoma among people working with animals or in meat-processing for some time but meat consumption has not been connected with transmission of oncogenic viruses yet. However, studies have found a lower risk of non-Hodgkin lymphoma in women consuming well-done meats instead of rare or rare-medium meats (Chiu et al., 1996; Zhang et al., 1999). So you are damned if you cook it, and damned if you don’t!
Summary
Stomach cancer is the fifth most common cancer worldwide. Processed meat is associated with an increased risk; just 30g a day (half an average serving) increases the risk by 15-27 per cent. People eating the most bacon have a 37 per cent higher risk than those eating the least.
In 2015, the WHO reported links between processed meat and stomach cancer. Then in 2016, the WCRF published a report saying that that there is now strong evidence that processed meat increases the risk of stomach cancer. They also said that some evidence suggests consuming grilled or barbecued meat and fish increases the risk of stomach cancer too. They blame high levels of salt, nitrite and nitrate (that can lead to the production of harmful NOCs) as well as carcinogenic and mutagenic PAHs, haem iron and salt.
So many factors may be at play, contributing to an increased risk of stomach cancer but avoiding meat (especially processed meat) is a simple choice you can make to protect yourself.
Stomach cancer – also known as gastric cancer – is the fifth most common cancer worldwide. Around 7,000 people are diagnosed with it each year in the UK (NHS Choices, 2015c). Unfortunately, as stomach cancer isn’t often picked up until the later stages, the outlook isn’t as good as for some other cancers. In the UK, around 5,000 people die from stomach cancer each year.
We have known about the links between processed meat and stomach cancer for over a decade. Even small amounts increase the risk and the more you eat, the bigger the risk. A 2006 review of 15 studies (including 4,704 stomach cancer patients) found that consuming just 30g per day (half an average serving) of processed meat increased the risk of stomach cancer by 15-27 per cent (Larsson et al., 2006). Seven of the studies specifically looked at the effect of bacon and found those eating the most had a 37 per cent higher risk of stomach cancer compared to those eating the least. They concluded that increased consumption of processed meat is associated with an increased risk of stomach cancer.
In 2015, the WHO announced that red and processed meat increases the risk of bowel cancer. They also reported links between red meat, pancreatic cancer and prostate cancer and processed meat and stomach cancer (WHO/IARC, 2015a). Then in 2016, the WCRF published a report from their Continuous Update Project – the world’s largest source of scientific research on cancer prevention and survivorship through diet, weight and physical activity (WCRF/AICR, 2016). They analysed worldwide research on how certain lifestyle factors affect the risk of developing stomach cancer. The report included new studies as well as those included in their 2007 report (WCRF/AICR, 2007).
For the first time, drinking alcohol, eating processed meat and being overweight were linked to an increased risk of developing stomach cancer. They said that there is strong evidence that consuming processed meat increases the risk of stomach cancer. Processed meat was defined as meat having undergone salt-preservation, smoking or fermentation, including sausages, bacon, ham, meatballs, burgers, cold meats and hot dogs. The report also said that some evidence suggests consuming grilled or barbecued meat and fish increases the risk of stomach cancer too.
How meat might cause stomach cancer
Potential mechanisms discussed in the WCRF/IARC report included the high levels of salt, nitrite and nitrate that many processed meats contain. Nitrite and nitrate from processed meat may be involved in carcinogenesis, due to reactions they trigger in the body. In the stomach in particular, nitrite and nitrate from meat can react with the degradation products of amino acids from meat to later form NOCs in the gut which are known carcinogens. Smoked meat is also often salted or cured, meaning that it is likely to raise endogenous production of NOCs. Smoked meat may also contain carcinogenic and mutagenic PAHs, depending on the fuel burned to produce the smoke.
A further potential mechanism linking processed meat intake to stomach cancer described in the report was haem iron which, as already stated, contributes to endogenous formation of NOCs, causes oxidative stress and DNA damage. Dietary iron has been identified as a growth factor for the bacteria Helicobacter pylori, an established risk factor for ulcers, inflammation and stomach cancer (Ward et al., 2012). Finally, the salt included in cooking, processing and preserving meat can damage the gastric mucosa (the stomach lining) and lead to inflammation (WCRF/IARC, 2016).
A study from Nebraska investigating the role of haem from meat in stomach cancer found the link with endogenous NOCs was present only among people infected with H. pylori and those with relatively low blood levels of vitamin C (Ward et al., 2012). The WCRF/IARC report found evidence that consuming little or no fruit increases the risk of stomach cancer and that consuming citrus fruit may decrease the risk of stomach cancer (WCRF/IARC, 2016). So it seems that many factors may work in combination contributing to an increased or decreased risk of stomach cancer but avoiding meat (especially processed meat) is a simple choice you can make to protect yourself.
To find out about the foods that fight cancer (fruit, vegetables, wholegrain foods, pulses, healthy fats in nuts and seeds) please see The Incredible Vegan Health Report.




